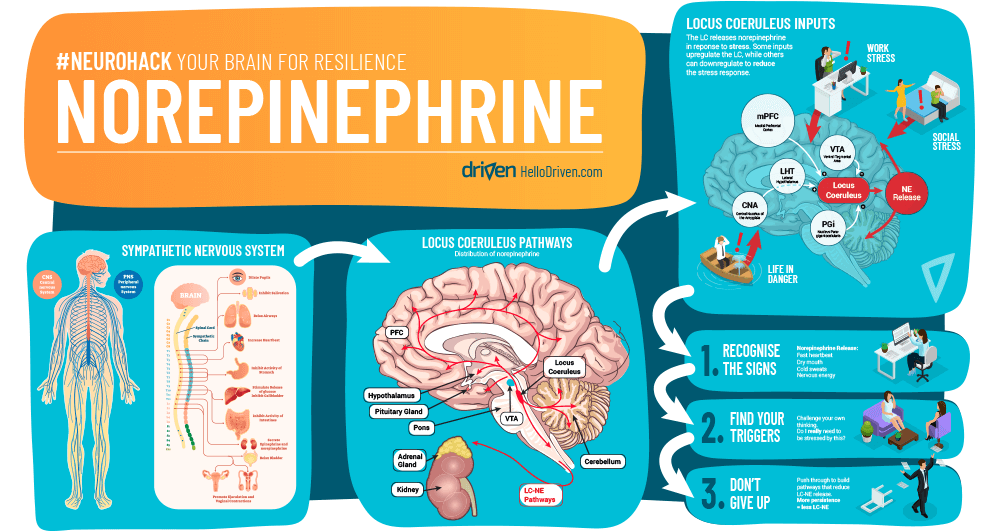
Your heart jumps and you suddenly become excruciatingly aware of a little too much perspiration. Words struggle to form in your mouth as you attempt to answer an unexpectedly tough question in the monthly project meeting you’re hosting.
Well hey there, norepinephrine! How nice to see you again…
What you’re feeling is the very noticeable effects of sudden neurochemical changes, like our old friend norepinephrine.
In Neurohack we will find new ways to boost your resilience by getting to know neurochemicals that affect your mindset. We’ll start by exploring norepinephrine, a key molecule involved in the fight-or-flight (or freeze) response.
Improve your persistence and build resilience with the Driven app. Download now.
The Bee’s NE
Also called noradrenaline, norepinephrine is similar (but different) to its more famous cousin epinephrine (adrenaline). To cut down on the big words, let’s shorten norepinephrine to NE.
NE has wide-ranging effects on both your physical and mental state – so effective regulation is very important for your capacity to be resilient.
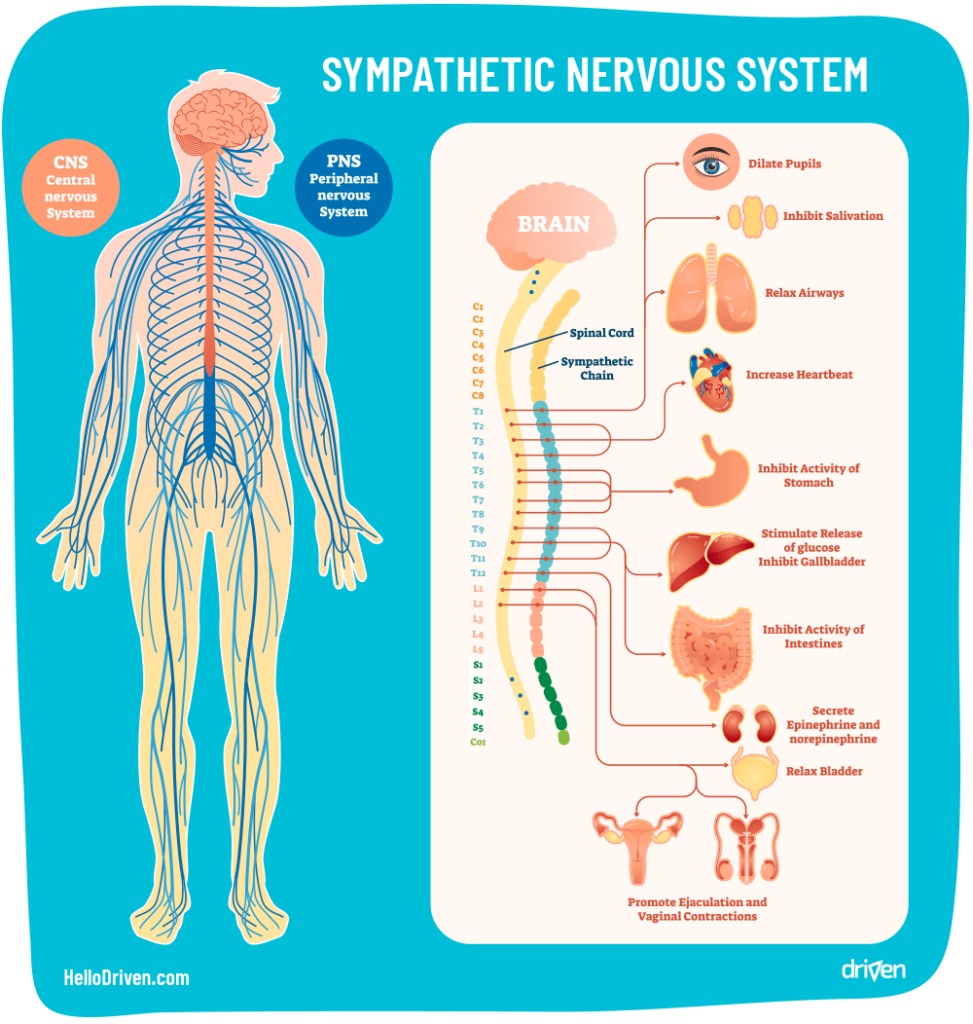
Sudden NE release affects you physically through the sympathetic nervous system (SNS). This is the system that tries to get you ready to survive a life-threatening situation, and is a major effector of the fight-or-flight response. Here are some of the physical changes from NE released through the SNS.
Pupils dilate, increased production of tears
Sweat secretion is stimulated
Increased heart rate
Increased calories burnt from brown adipose tissue
Changes to immune system
Arteries are constricted to increase blood pressure
Glucagon production in the pancreas is increased
Glucose production in the liver is increased
Glucose uptake in skeletal muscles is increased
Reduction of digestive activity in stomach and intestines
To start off nice and easy, you might remember this diagram below from school days.
With so many effects, it’s little wonder why even insects like bees have NE in their venom[i]. It helps them take advantage of the many neurochemical receptors in the body that respond to NE, allowing for an increase in the potency of the venom.
Neurotransmitter, or Hormone?
When NE is released through the SNS, it is a neurotransmitter. However, one of the effects of NE release is to stimulate further NE release from the adrenal glands that sit on top of the kidneys. When NE is released from there, it is released as a hormone.
Although it’s still the same molecule, it is classified differently based on where it is released. Thinking from a resilience perspective, the mental aspect is more interesting; therefore we’ll look a bit more closely at its role as a neurotransmitter. Why? Well, the physical symptoms are certainly a good indicator that NE is being released, but it’s the impact on our mindset that we really feel, and is also what we can do something about.
NE Effects on the Mind?
It’s in the brain itself where we can see the true impact of NE. In fact, NE is increasingly emerging as a key mediator of some of the most prevalent mental disorders, including social anxiety disorder, general anxiety disorder, PTSD, depression, and even Alzheimer’s[ii].
To see just how NE can be this powerful, we need to find the source – the locus coeruleus (LC). Latin for ‘blue spot’, the LC sits in the back of the pons and gains its characteristic blue colour from the polymerisation process (creation) of NE.
The LC likes to be connected. It is part of a group of brain structures called the reticular activating system (RAS). Together, these structures control states of consciousness, sleep-wake transitions, and focuses attention.
From its position around the middle of the RAS, the LC projects widely into many other structures. These projections (and effects) include:
Cerebral cortex (reduce higher thinking)
Amygdala (increase threat detection & memory formation)
Cerebellum (movement & multitasking)
Brain stem & spinal cord (SNS activation)
Hypothalamus (activation of fight-flight response)
Tectum (increases visual & auditory reflexes)
Thalamus (focuses attention)
Ventral tegmental area (inhibits dopamine production)
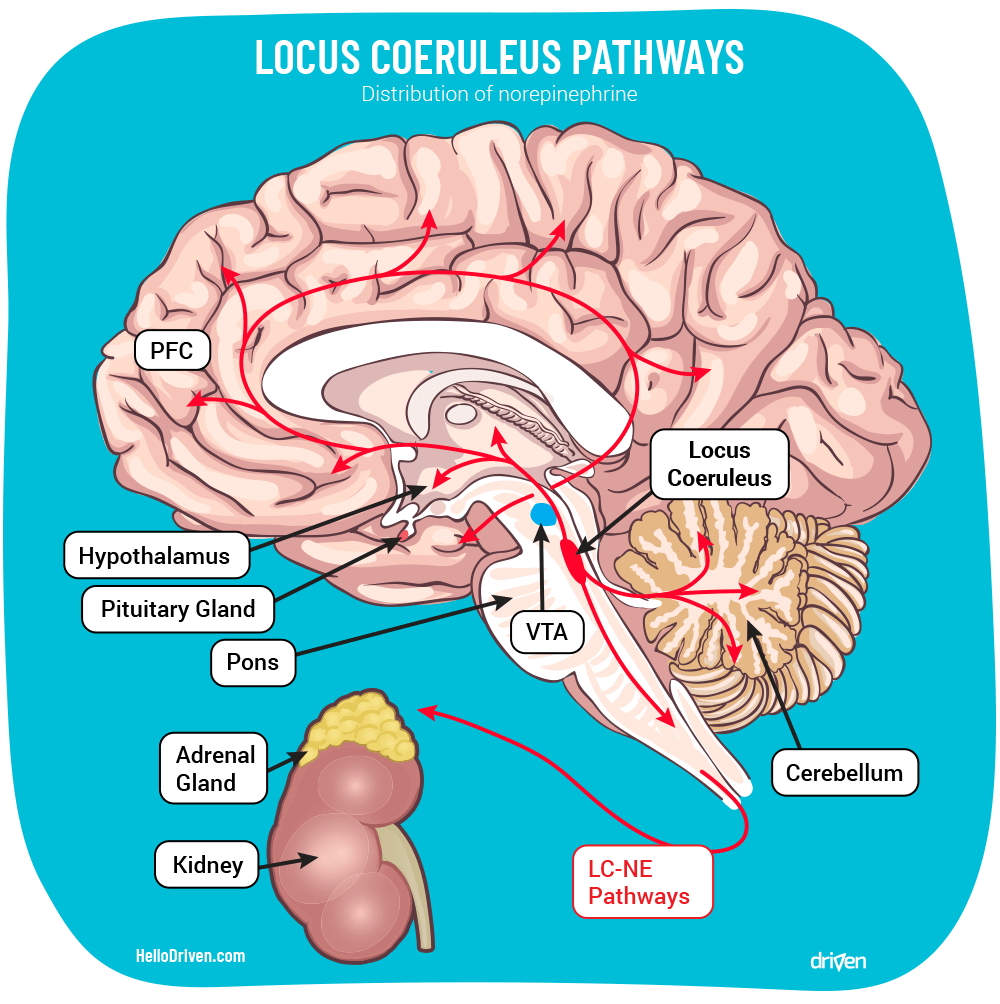
As you can see, the locus coeruleus norepinephrine (LC-NE) projections affects a large number of areas, including – to a large extent – your essential experience of consciousness. No wonder it is found to play such an important role in many disorders, and why its effective functioning is a critical target for resilience.
The effect of NE on the ventral tegmental area (VTA) is quite important, as the VTA where the dopaminergic neurons originate. The VTA neuros distribute dopamine throughout the brain using two key neural ‘highways’ called the mesolimbic and mesocortical pathways.
Dopamine is often misunderstood as a ‘feel-good’ molecule. In reality, it is a motivator. It motivates us to take some kind of action that might have some reward at the end. Therefore, dopamine is released in anticipation of a reward. This anticipation is what motivates us to do something, rather than nothing.
But what does this feel like?
Low motivation – Constant LC-NE activation reduces VTA function, resulting in lower dopamine release, and therefore lower levels of motivation. At higher levels of LC dysregulation, depression can occur[iii].
Tunnel vision – You gain a kind of tunnel vision, focusing on narrow aspects while avoiding the larger implications of your actions.
Anxious – Dry mouth, cold sweats, nervous energy… These are all symptoms of LC-NE activation that underlies feelings of anxiety.
One of the challenges is that the brain’s fear system is not so great at distinguishing life-threatening stress from non-life-threatening stress. This means we often experience more NE release than is helpful, so learning about ways to bring this under control is important for our mental wellbeing!
LC Activators
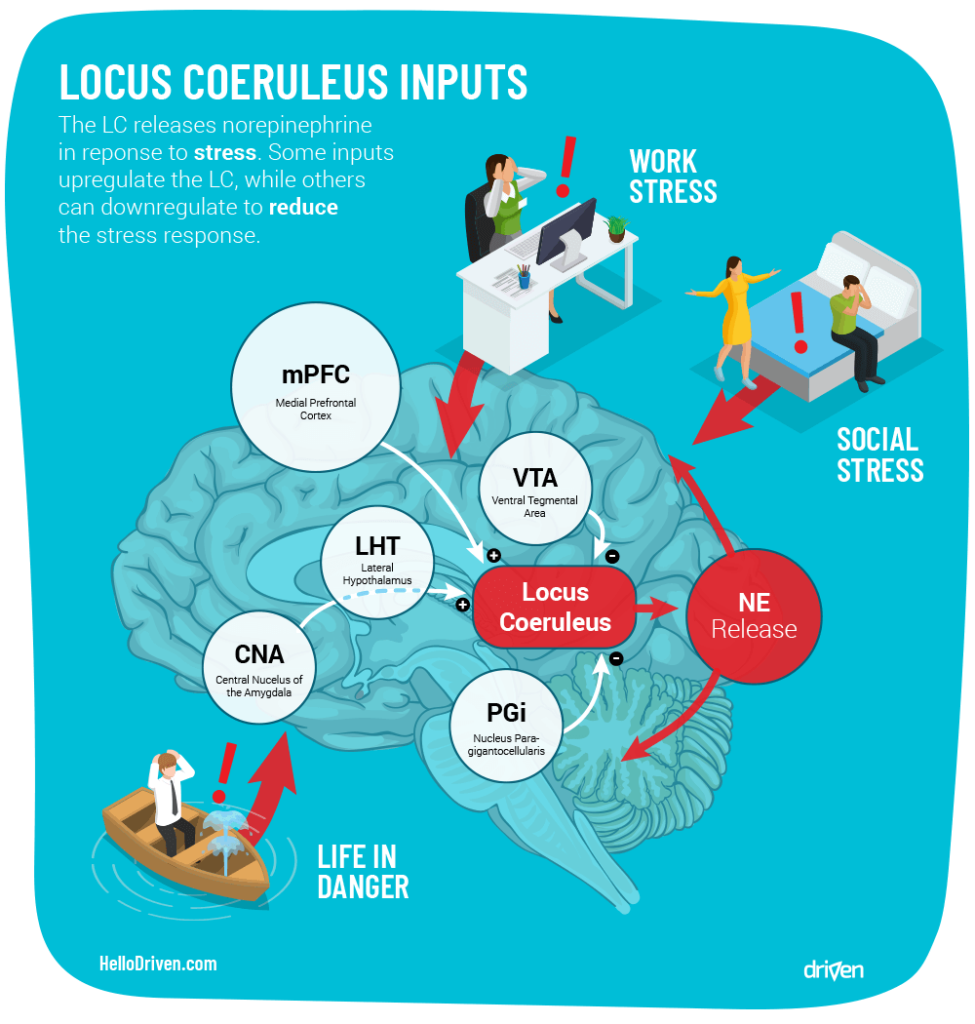
What causes LC-NE activation in the first place? Quite simply, stress. This can originate from a few different places, so let’s meet the top players that input to the LC.
Medial prefrontal cortex (mPFC) – This area is involved in establishing contextual associations between locations, events and responses[iv]. It helps us understand what is appropriate in different social settings, and associates emotional responses with these settings as well.
The mPFC’s role therefore makes it quite clear how it plays a role in social anxiety – uncertainty or stress associated with social settings result in the LC to be activated, resulting in NE release and all its resulting unpleasant effects, just when you need it least.
Recent research revealed how persistence (resisting giving up) in social stress situations builds resilience
Ventral tegmental area (VTA) – We’ve already seen that the LC has the ability to reduce activation of the VTA, resulting in lower motivation and potentially phenomenological depression. However, connections from the VTA to the LC have also been found[v].
These connections show that the VTA can release dopamine within the LC, resulting in reduced NE expression. Here we see the brain’s capacity to develop regulatory circuits to manage its own internal connection in complex ways.
Interestingly, many selective serotonin reuptake inhibitors (SSRI, like fluoxetine – Prozac, or escitalopram – Lexapro) assists with LC regulation which helps alleviate depressive symptoms. Considering the direct role of the VTA and LC in depression, dual acting anti-depressants such as a norepinephrine-dopamine reuptake inhibitor (NDRI, like bupropion – Zyban) have the ability to directly impact regulation of these areas and have been suggested by some researchers as intervention for treatment-resistant depression[vi].
Nucleus paragigantocellularis (PGi) – I promise I’m not just making up words here. Sitting a bit lower from the LC in the medulla, the PGi has the ability to inhibit the activation of the LC through the release of enkephalins (internally produced opioids)[vii].
Recent research revealed that persistence (resisting giving up) in social stress situations builds stronger connections between the PGi and the LC, allowing the PGi to reduce NE release by the LC. Quite simply, resisting defeat builds resilience.
Lateral hypothalamus (LHT) – Following on from the PGi, what we see from the research is that when we give up too soon, it means that there are strong connections from the LHT to the LC. These connections originate from the central nucleus of the amygdala (CNA), carrying corticotropin-releasing factor (CRF) which activates the LC[viii].
When we are prone to give up, these connections strengthen, meaning more NE is released and we become more easily stressed. Eventually, the research shows that this give-up coping strategy results in lower motivation, eventually leading towards symptoms of depression. This has been seen elsewhere by studies that have linked depression to LC activation[ix].
Do We Want Less NE?
From what we’ve said so far, it could seem like less NE is better. However, like with most things in the brain, it’s never quite so simple. Things in the brain are so heavily connected that when you think you’ve just fixed one problem, you’ve created two more elsewhere.
I subscribe to a simple belief – humans have the power to improve any aspect about themselves.
For example, NE has some anti-inflammatory purposes too, helping to keep certain areas in the brain ‘clean’. Also, too little NE release makes it hard to focus on something, resulting in too much daydreaming[x]. This is due to the default mode network DMN that usually activates when you sit down on the toilet (seriously). While DMN activation is a great source of creative thinking, it does become a bit problematic when you can’t focus long enough to put those eureka moments into practice, aka ADHD[xi].
So the key for your brain is effective regulation of the LC-NE system, enabling enough NE to keep you focused and productive, but not too much that it makes you feel stressed and anxious.
What Can You Do?
I subscribe to a simple belief – humans have the power to improve any aspect about themselves.
This is the basic belief of mine that underscores all the work I do in the field of resilience – learning about the brain and human nature so that I can find ways to help people change and build deep resilience.
Learning from when we’ve explored about NE, here are three ways you can regulate the LC-NE system.

1. Recognise the signs
In the short term, the easiest strategy you can learn is to quickly recognise the signs of NE release. These include dry mouth, increased sweat, faster heartbeat, and that feeling of nervous energy.
Your PFC has an amazing ability to override these moments and tell your brain that it is safe and it doesn’t need to panic. How do you do this? Breathe. Simple slow breathing has the ability to calm your LC-NE system so that you can regain your calm.
Key PR6 Skill – Composure

2. Find your triggers
This can be challenging, but it’s also the more rewarding in the long term. It’s about finding what triggers your NE release and then challenging yourself to think differently about those times.
For example, does your LC-NE system go into overdrive when you are in traffic? Then try building compassion for other drivers, accept they are not perfect, and focus instead on listening to some music or a podcast.
There are many situations like this that causes stress, but really doesn’t need to. By challenging yourself to behave differently, you start to build connections in the brain the downregulates LC activation, helping you stay resilient and deal with these situations with ease.
Key PR6 Skill – Reasoning

3. Don’t give up
When you face challenges, persist.
As you persevere, you build stronger connections between the LC and the PGi. This means you develop a stronger ability to regulate LC-NE release, meaning you start to experience less stress when facing challenges, and you can work through them with more confidence.
This starts with a simple decision to not give up when things get tough. From there, it’s about summoning the courage to keep going and keep trying until you succeed.
Key PR6 Skill – Tenacity
Conclusion
Norepinephrine is a major neurochemical that features every day in your experience of life. It affects your decision-making processes, motivation, attention, and much more.
Fortunately, there are ways you can influence NE release, effectively allowing you to do some neurohacking to build your own resilience.
Well, we got a bit technical here, but in the end I think the lessons mean much more if you know how things work. What do you think? Would you like more articles like this? If so, comment, share & like the article and I’ll get writing on the next one! Any suggestions on which neurochemical to focus on next?
All the best,
Jurie
[i] Sahinkus S, Demirel S, ÖskeN A, Gunduz H, Akdemir R (2017) Atrial Fibrillation Due to Bee Sting. J Clin Toxicol 7: 361. Doi: 10.4172/2161-0495.1000361
[ii] Ressler, K. J., & Nemeroff, C. B. (2001). Role of norepinephrine in the pathophysiology of neuropsychiatric disorders. CNS spectrums, 6(8), 663-670.
[iii] Weiss, J. M., Boss-Williams, K. A., Moore, J. P., Demetrikopoulos, M. K., Ritchie, J. C., & West, C. H. (2005). Testing the hypothesis that locus coeruleus hyperactivity produces depression-related changes via galanin. Neuropeptides, 39(3), 281-287.
[iv] Euston, D. R., Gruber, A. J., & McNaughton, B. L. (2012). The role of medial prefrontal cortex in memory and decision making. Neuron, 76(6), 1057-1070.
[v – vi] El Mansari, M., Guiard, B. P., Chernoloz, O., Ghanbari, R., Katz, N., & Blier, P. (2010). Relevance of norepinephrine–dopamine interactions in the treatment of major depressive disorder. CNS neuroscience & therapeutics, 16(3), e1-e17.
[vii – viii] Reyes, B. A., Zitnik, G., Foster, C., Van Bockstaele, E. J., & Valentino, R. J. (2015). Social stress engages neurochemically-distinct afferents to the rat locus coeruleus depending on coping strategy. eNeuro, ENEURO-0042.
[ix] Weiss, J. M., Boss-Williams, K. A., Moore, J. P., Demetrikopoulos, M. K., Ritchie, J. C., & West, C. H. (2005). Testing the hypothesis that locus coeruleus hyperactivity produces depression-related changes via galanin. Neuropeptides, 39(3), 281-287.
[x] Unsworth, N., & Robison, M. K. (2017). A locus coeruleus-norepinephrine account of individual differences in working memory capacity and attention control. Psychonomic bulletin & review, 24(4), 1282-1311.
[xi] Silberstein, R. B., Pipingas, A., Farrow, M., Levy, F., & Stough, C. K. (2016). Dopaminergic modulation of default mode network brain functional connectivity in attention deficit hyperactivity disorder. Brain and behavior, 6(12), e00582.